And What Are We Going To Do About It? Read On!
Written By Anna M. Cabeca, DO
October 3, 2003
With so much news about breast cancer and the ever-present danger of having it, getting it, and knowing someone we love and care about with it, we all do our breast exams, and keep up with our mammograms, and remind a buddy, Right? I WISH!
Truth be told, less than 10 % of us actually keep up with our own health, let alone anyone else’s. Possibly, we think that if I don’t think about sickness, cancer, disease, health, then I am not going to get sick, it is not going to happen to me, or I’ll just ignore it and it will go away. But we are wrong again. With this article, I hope to persuade a few more percents to be proactive in not only our own health but those of our families, friends, neighbors, pets, etc. Get the point?.
First, to bring this home to us and further understand our own risks, let us review risk factors for developing breast cancer.
- Prior breast cancer. If you have ever had it, please keep up with your examinations. Also having had a breast biopsy that showed “lobular carcinoma insitu” and “atypical ductal hyperplasia” put you at higher risk.
-
Genetics and Family history : The lifetime risk of being diagnosed with invasive breast cancer is about one in eight for women, but is about two to three times greater for women with a history of breast cancer in a first-degree relative (mother, sister, or daughter) than in women with no family history of breast (or ovarian) cancer. Only 9% of breast cancer can be attributed to a “family history” of breast cancer and fewer associated with a hereditary gene or germ cell mutation, i.e. the BRCA1 and BRCA2. There is a higher association between breast, ovarian, and colon cancers. Therefore your personal risk is increased by:
- having a mother, sister, or daughter with breast cancer
- having multiple generations of family members affected by breast or ovarian cancer,
- having relatives who were diagnosed with breast cancer at a young age (under 50 years old),
- having relatives who had both breasts affected by cancer.
- Environmental Factors: 90% of breast cancers are attributed to various environmental factors such as:
- Exposure to ionizing radiation
- Exposure to DDT and contaminants of pesticides (this research has been inconsistent)
- Smoking and second-hand smoke
- Obesity, especially adult weight gain
- High-fat diets
- Alcohol use
- Older age of first child’s birth and never having a child
- Later menopause
- Also, the risk of prolonged hormone replacement therapy in menopausal women on Premarin and Provera has been shown to increase the risk by 8 per 10,000 women.
We can come to grasp our individual risk as 1 in 8 women in my lifetime. So, let’s now talk about PREVENTION, DETECTION, and DIAGNOSES of breast cancer.
PREVENTION: The best medicine and the best doctor are able to prevent disease. Here is what we know about breast cancer prevention. It begins with strengthening your immune system. Follow this advice and you will not only help to reduce your risk of breast cancer but hopefully prevent it and many other illnesses, too.
- If you smoke – QUIT!! – I often tell my patients, if I could think of one good thing about smoking I would tell them, but I can not. NO! NO! NO! QUIT!
- Exercise 30 minutes 5 days per week.
- Drink plenty of water, good old H2O! 8 to 10 glasses per day to keep our body fluid and flush toxins
- Eat your vegetables!!! Squash, carrots, tomatoes. These contain carotenoids that fight disease.
- Eat Salmon, olive oil, lean meats, don’t fry. Foods in their natural form have many “anti-oxidants” that help our body fight off “free radicals” that promote disease.
- Supplement your diet with Vitamins E, C, Omega-3. Again, these are powerful anti-oxidants that have favorable effects on our immune system to fight off disease.
- Stop drinking alcohol or limit to 4 oz of red wine per night (begun after you begin your meal).
- Avoid foods that may have stored hormones or pesticides.
- Shed those extra pounds and work hard to keep them off and maintain your goal weight.
- Tamoxifen and Raloxifene are in ongoing studies evaluating their role in the prevention of breast cancer.
- BE MINDFUL! Our bodies are given a special power to heal and take the opportunity each day to invoke that. Some ways that you can do this is:
- Prayer
- Meditation
- Yoga
- Laughter
- Talking
- Sharing
- Loving
Anything that you can do to enhance your joy of life and relieve your stress to give back your body its maximum power to heal itself.
DETECTION and SELF-EXAM: Great, so now you are taking a proactive role in your health and are ready to learn about the detection of breast cancer. The key to treatment is early detection.
1. Mammograms. The American Cancer Society has established guidelines on screening mammograms. While mammograms do not prevent breast cancer, they can save lives by detecting early disease. Mammograms have been shown to lower the chance of dying from breast cancer by 35% in women over 50 years old.
We currently recommend a baseline mammogram at age 35 years old for women and then yearly after age 40 years old. Mammograms are not perfect, however, and dense breast tissue can sometimes mask true disease. If you or your doctor feels a lump or see an abnormality on self or physician exam, be persistent. You are your best advocate. Sometimes diagnosis requires additional views by mammogram, breast sonogram, or a needle biopsy.
2. Breast Self Examination.
Step 1: The first step to breast self-exam is always visual inspection. Yes, this requires looking at your body naked in the mirror. Raise your hands above your head and look for any pulling or dimpling of the skin or inversion (pulling in) of the nipple. Look at any changes to skin color, redness, swelling, change in nipple direction, or a lump.
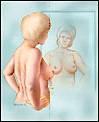
Step 2: Keep looking, now push your hands together over your head and then bring your arms down and push in at your waist using your chest muscles. This contracts the pectoral muscles. If a tumor is growing under the skin it will attach from the connective tissue over the muscle to the connective tissue under the skin. Let your doctor know if there is any change, dimpling, irregularity in the skin.
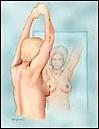
Step 3: While seated or standing in the shower (soapy wet skin makes it easier to feel), examine your breasts with one hand over your head, feel with the opposite hand above your clavicle and under your arm for any lumps, bumps, irregularities, tenderness, and note any discharge. It is best to use the soft pads of your three middle fingers and use soft, medium and deep pressure. Be sure to examine the whole breast, from under the arm to the midline of your chest, then change sides and do it again. You can use a circular motion, up and down, left to right, it does not matter as long as you are consistent and do your exams the same way each time, and you will detect a difference should a problem occur.
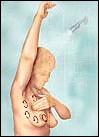
Step 4: Finally lay down, take your time and repeat the breast exam as you did when standing.

Step 5: Report any abnormal findings to your doctor and follow up! This leads us to physician examination.
PHYSICIAN EXAMINATION: Your physician should examine your breasts yearly and take you through the same steps as above, inspection, exam seated and lying. Any abnormalities are usually followed up with a mammogram, ultrasound, and or biopsy as described above. These appointments are important and please follow up with them. Your doctor may feel or see something you do not. Some patients have twice yearly or more frequent exams with their physician based on personal and family history.
Always discuss with your doctor any concerns or questions you may have. Write them down before you go into the office so you will not forget. Take an active role in your healthcare and your families.
October is Breast Cancer Awareness Month – spread the word! I hope you find this advice useful and will take these steps to create the healthiest you possible!
Sincerely,
Anna Cabeca, DO




